Ocular Hypertension
Ocular Hypertension
Ocular hypertension is when the pressure inside the eye (intraocular pressure or IOP) is higher than normal.
Eye pressure is expressed in millimetres of mercury (mm/Hg), the same unit of measurement used in weather barometers. While normal eye pressure has historically been considered a measurement of less than 21mm/Hg, this normal "normal" upper limit may vary in different populations.
Ocular hypertension is not the same as Glaucoma, which is a disease of the eye often caused by high intraocular pressures. In people with ocular hypertension, the optic nerve appears normal and no signs of Glaucoma are found during visual field testing, which tests side (peripheral) vision. However, people with ocular hypertension are considered "Glaucoma suspects", meaning they should be monitored closely by an Ophthalmologist to make sure that they do not develop Glaucoma.
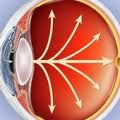
Ocular Hypertension Causes
In the healthy eye a clear fluid called aqueous humor circulates inside the front portion of your eye. To maintain a constant healhty eye pressure, your eye continually produces a small amount of aqueuous humor while an equal amount of this fluid flows out of your eye.
Injury to the eye can cause ocular hypertension, as can certain eye diseases. Certain medications (such as steriods) are also a potential for cause for ocular hypertension.
While anyone can develop ocular hypertension, the follwing people are at greatest risk for this condition:-
- People with a family history of ocular hypertenstion or Glaucoma
- People with diabetes
- People over age 40
- People of African American descent
- People who are very myopic (nearsighted)
Ocular Hypertension Symptoms
Ocular hypertension usually does not have any signs or symptoms. Because you can have ocular hypertension and may not be aware of it, it is important that you have regular eye examinations.
Ocular Hypertension Diagnosis
As part of a comprehensive eye examination, Mr. Golchin will perform tests to measure your intraocular pressure and to make sure that you do not have Glaucoma.
Below is a list of tests that may be performed:-
Tonometry Exam.
This procedure measures the pressure in your eye. During this exam, your eyes are numbed with eye drops. Mr. Golchin uses an instrument called a tonometer to measure eye pressure. The instrument measures how your cornea resists to pressure.
Gonioscopy Exam.
Gonioscopy allows Mr. Golchin to get a clear look at the drainage angle of your eye. Mr. Golchin is not able to see your eyes drainage by looking at the front of your eye, however by using a mirrored lens, he can examine the drainage angle, which is important in determining whether or not you have Glaucoma, as well as what type of Glaucoma you may have.
Ophthalmoscopy Exam.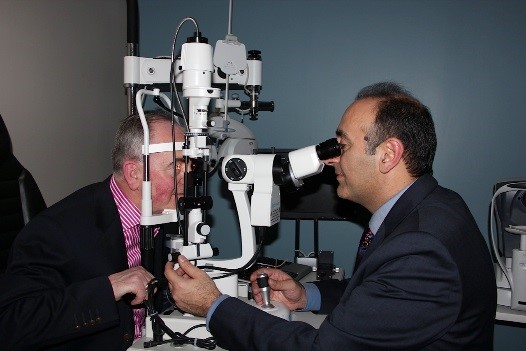
Your optic nerve is inspected for signs of damage using an ophthalmoscope, an instrument that magnifies the interior of the eye. Your pupils will be dilated (widened) with eye drops to allow a better view of your optic nerve to see if it is has been damaged.
Visual Field Test
The visual field test will check for blank spots in your vision, another sign of Glaucoma. The test is performed using a bowl shaped instrument called perimeter. When taking the test, a patch is temporarily placed on one of your eyes so that only one eye is tested at a time. You will be seated and asked to look straight ahead at a target. The computer makes a noise and random points of light will flash around the bowl shaped periemter and you will be asked to press a button whenever you see a light. Not every noise is followed by a flash of light.
one of your eyes so that only one eye is tested at a time. You will be seated and asked to look straight ahead at a target. The computer makes a noise and random points of light will flash around the bowl shaped periemter and you will be asked to press a button whenever you see a light. Not every noise is followed by a flash of light.
Pachymetry
Because the thickness of the cornea can affect eye pressure readings, pachymetry is used to measure corneal thickness. A probe called a pachymeter is gently placed on the cornea to measure its thickness.
Ocular Hypertension Treatment.
It is important to monitor ocular hypertension closely and to reduce it before it causes vision loss or damage to the optic nerve. Depending upon your individual case and how high your intraocular pressure is found to be, Mr. Golchin may not decide to initiate treatment immediately but instead monitor your intraocular pressure through regular scheduled testing.
In other cases Mr. Golchin may decide that medication is needed to reduce your intraocular pressure. Pressure lowering eyedrops can improve your ocular hypertension but it is important for you to adhere to your prescribed regimen for them to work effetively.
In some cases you may be prescribed more than one medication. When prescribing medication, Mr. Golchin will schedule a visit within several weeks to test your eye pressure again in order to determine how effective the medication is in treating your ocular hypertension.
Mr Golchin may also decided to perform SLT (Selective Laser Trabeculoplasty) to reduce your Intraocular pressure.
Many patients with ocular hypertension may go on to devleop primary open angle Glaucoma which almost always requires therapy to lower intraocular pressure.






 one of your eyes so that only one eye is tested at a time. You will be seated and asked to look straight ahead at a target. The computer makes a noise and random points of light will flash around the bowl shaped periemter and you will be asked to press a button whenever you see a light. Not every noise is followed by a flash of light.
one of your eyes so that only one eye is tested at a time. You will be seated and asked to look straight ahead at a target. The computer makes a noise and random points of light will flash around the bowl shaped periemter and you will be asked to press a button whenever you see a light. Not every noise is followed by a flash of light.